Keratoconus

Keratoconus is a progressive eye disease which affects the shape of the cornea causing blurred vision. In 20%-30% of cases, the condition is progressive resulting in thinning and weakening of the cornea. This then causes the cornea to bulge into a cone-like irregular shape causing distorted and blurred vision.
What is keratoconus?
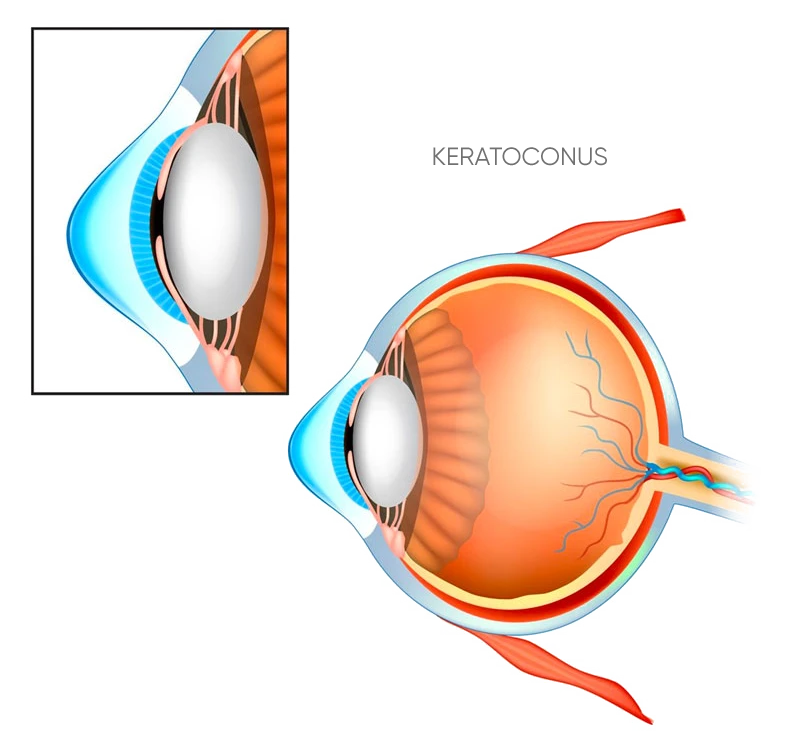
Keratoconus is a progressive non-inflammatory condition of the cornea (the clear window at the front of the eye) which causes its shape to change and bulge. It is a condition which gets progressively worse and may eventually result in the splitting of the back surface of the cornea. This is known as acute corneal hydrops.
The bulging, cone-shaped cornea distorts the light that travels to the retina, resulting in distorted images being passed to the brain.
Clinical features of keratoconus
Keratoconus always affects both eyes, although there can be a marked difference in the severity of each eye affected. Optometrists sometimes pick up keratoconus due to an increase in the astigmatism of their patients. Increasing astigmatism should trigger a suspicion of keratoconus and referral for specialist investigation.
The astigmatism associated with keratoconus is not regular, which means that it cannot be fully corrected with glasses. In very mild/early cases people may see relatively well with glasses alone, although most people with more advanced keratoconus see best with special keratoconus contact lenses.
What are the symptoms of keratoconus?
Keratoconus affects around 1 in 2000 Caucasian and 1 in 500 Asian people.
The symptoms are blurring and reduced quality of vision, and can make tasks such as driving and reading difficult. You may also experience sensitivity to bright light, and ‘ghosting’ of images, particularly when driving at night. The symptoms may change over time.
Keratoconus causes vision to change frequently and if you find your lens prescription changes often, this could be a sign of keratoconus.
What are the causes of keratoconus?
The underlying problem is weakness of the supporting collagen fibres in the cornea. This makes the cornea structurally and biomechanically “weak”.
It mainly affects people in their teens through to their early thirties. It is most common in people with Down Syndrome, and in people of Asian or Middle Eastern ethnicity. It can also affect people with asthma or eczema. It affects males and females equally, and can effect one eye more than the other.
- Hereditary factors
- Allergies
- Eye rubbing
How is keratoconus diagnosed?
If you are experiencing poor quality of vision, speak to your optician or contact us for an appointment. Keratoconus can be similar to astigmatism and is often picked-up during astigmatism consultations.
Keratoconus can be diagnosed using state of the art elevation-based scheimpflug corneal topography. This technology also allows detection of subclinical forms of keratotoconus, such as forme fruste keratotoconus. It also allows the keratoconus to be quantified, so that your surgeon can let you know if and at what rate your condition is progressing. This is very helpful in deciding keratoconus treatment options.
Keratoconus can take many years to develop and regular check-ups are recommended for anyone diagnosed with this condition.
What are the treatment options for keratoconus?
Mild cases of keratoconus can be treated through the use of glasses and specialist contact lenses. In more serious cases, a corneal implant or transplant may be needed. Up to 1 in 5 people with keratoconus will need surgery.
Most cases of keratoconus can be corrected with a range of specialist contact lenses, or a combination of corneal surgery and contact lenses. The disease generally stops getting worse in your 30s.
Keratoconus is a more serious eye condition but advances in technology mean that it can be treated and activities such as driving and reading are now possible for keratoconus sufferers. Keratoconus treatments have a high success rate and further research will increase this success even further still.
Surgical treatment options
Accelerated Corneal Collagen Crosslinking (CXL)
Corneal collagen crosslinking has revolutionised the management of keratoconus. Now, for the first time, there is a keratoconus treatment available that can stop the disease from progressing.
The procedure is done as a day case under topical anaesthetic drops. The cornea is soaked in Riboflavin (vitamin B2) drops and then an ultraviolet light (UVA) is shone onto the cornea. With traditional crosslinking, this keratoconus treatment takes an hour, but with accelerated crosslinking, the procedure can be done safely in a shorter time. A bandage contact lens is placed on the cornea at the end of the procedure and this is removed once healing is complete between 3-5 days after the treatment.
Want to know more?
Keratoconus is progressive, but its progression can be managed and slowed. Get in touch by phone, email or our online form.
Enquire today:
Unit 11, Building 7
49 Frenchs Forest Rd East
Frenchs Forest NSW 2086

